Khomotso matriculated in Lephalale in Limpopo and made her way to Bloemfontein in January 2014. She was determined to succeed in life and knew that she had one chance to achieve her objective, which was to obtain a degree. However, coming from a family with an annual income of less than R80 000 she knew she would have to find funding. She secured a bursary with Distell, although it would only cover her tuition, so her next challenge was finding funding for meals and other expenses.
Making a difference daily
When she arrived at the University of Free State (UFS) she applied for the No Student Hungry (NSH) Food Bursary through the Social Work Services office and was successful. The weekly NSH funds she received enabled her to buy food and offered her extra opportunities to develop herself through student wellness workshops. NSH funded her for the next three years. “It was a relief not to worry about where my next meal would come from, allowing me time to concentrate on my studies,” said Khomotso.
Three years later she graduated with 22 distinctions and is pursuing her postgraduate studies in Education in 2018. For her, it is important to create the change that our country needs. “It was my teachers and parents who inspired me to pursue a degree. As a future teacher, I want to be able to make a difference in the lives of young people. “
Donors key in reducing food insecurity
Like Khomotso, there are many academically strong students who lack adequate financial support to sustain them through their degree programmes. For this reason, the financial contributions made to the NSH Food Bursary Programme by staff of the UFS, alumni and other donors remains crucial. Systemic change occurs when students graduate and join the country’s workforce. Together, we continue to cause ripples of change in our country.
The South African Surveys of Student Engagement Annual Report (2016) reflects that “it is clear that financial stress impacts on different areas of students’ lives. It is also clear that the impact is magnified for those who are already vulnerable, such as students who come from poor families”.
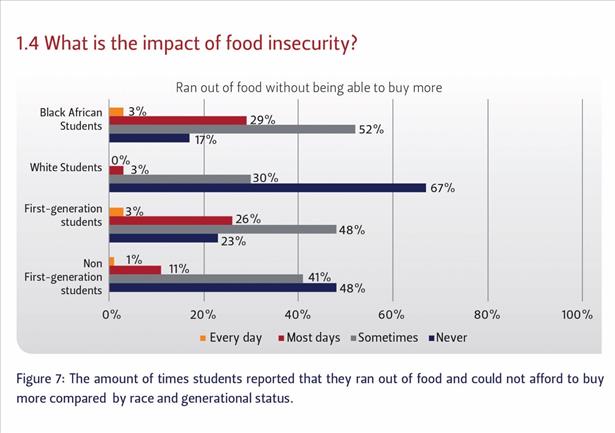
Figure 7 shows that 32% of black African students reported that they ran out of food and could not afford to buy more on most days or every day. Similarly, a significant difference in responses is seen between first- and non-first-generation students, with 77% of first-generation students indicating that they ran out of food without being able to buy more, compared to 53% of non-first-generation students.
The overall academic average of 2017 NSH students was 61% on all three UFS campuses, with the top 10 achievers of 2017 being females predominantly in the black African and coloured designated groups, in the fields of Communication, Law, Education, Science, Social Science and Psychology, scoring on average above 70%.
Give to the NSH Food Bursary.
Contact: Vicky Simpson, Officer Institutional Advancement SimpsonVZ@ufs.ac.za /call: +27 51 401 7197.